Top Features of HIPAA Compliance Monitoring Tools
Post Summary
HIPAA compliance tools are transforming how healthcare organizations protect patient health information (PHI). These tools streamline compliance through automation, real-time monitoring, and centralized management. Here's what you need to know:
- Real-Time Alerts: Instantly detect and address compliance issues like misconfigurations and access violations.
- Automated Evidence Collection: Save time by continuously gathering logs, training records, and encryption proofs.
- Risk Assessment Automation: Evaluate and manage risks efficiently with structured workflows and dynamic updates.
- Continuous Control Monitoring: Ensure security safeguards are always active and effective.
- Vendor Management: Simplify Business Associate Agreement (BAA) tracking and third-party risk assessments.
- Centralized Policy Management: Keep all HIPAA-related documents in one secure location.
- Audit Trails and Reporting: Generate audit-ready reports with detailed logs and compliance metrics.
These tools integrate with existing systems like EHRs and cloud platforms, reducing manual effort while improving compliance oversight. By automating key processes, healthcare organizations can focus on patient care while staying compliant with HIPAA regulations.

8 Essential Features of HIPAA Compliance Monitoring Tools
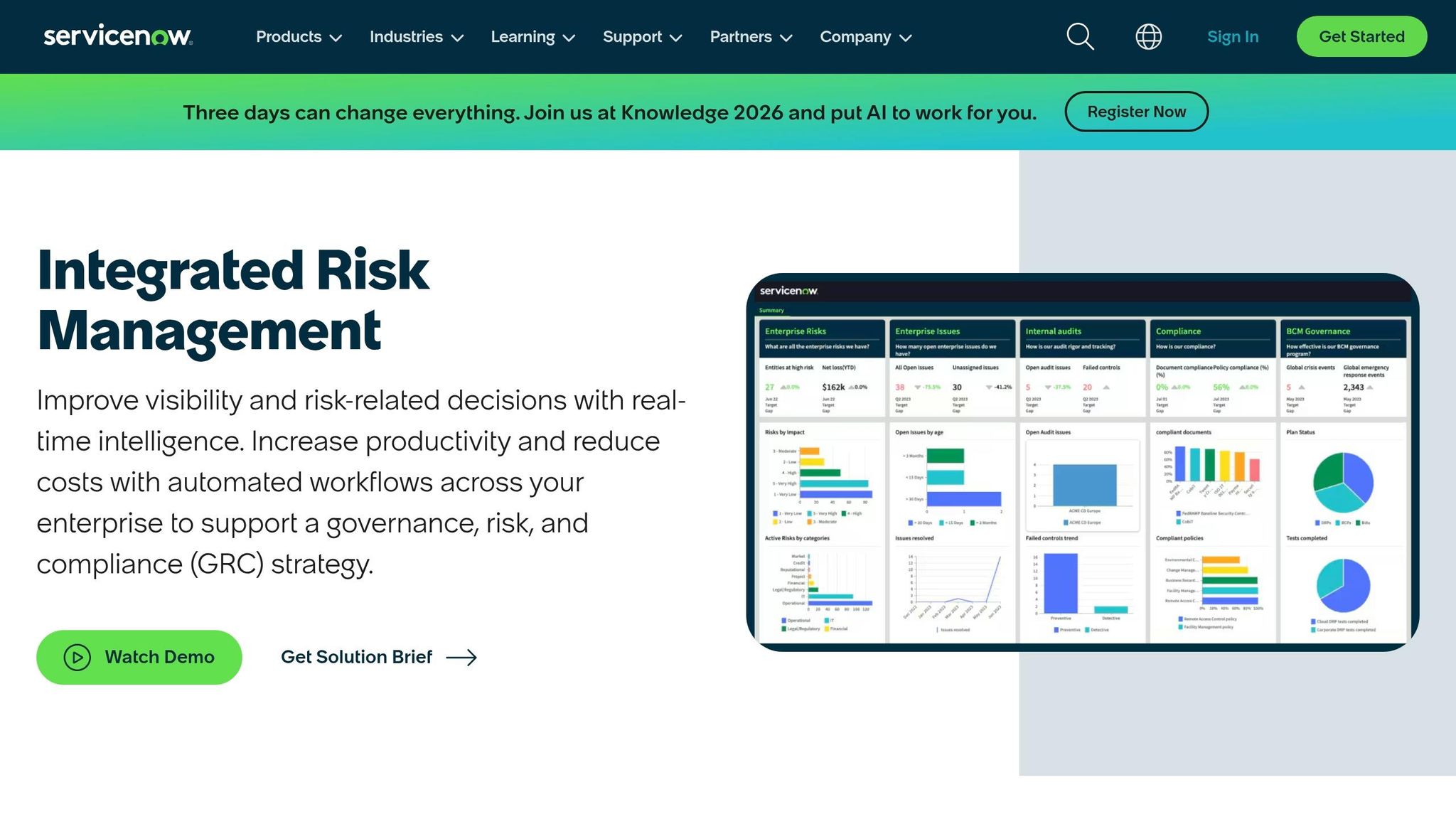
Quick wins to optimize HIPAA compliance management using ServiceNow IRM
sbb-itb-535baee
1. Censinet RiskOps™
Censinet RiskOps™ is a cloud-based platform tailored for healthcare organizations to manage cybersecurity and HIPAA compliance risks across their operations. Unlike traditional Security Risk Assessment (SRA) methods, this platform provides a centralized hub for overseeing risks to patient data, clinical systems, medical devices, and supply chains.
Real-time monitoring and alerts
The platform delivers real-time insights into compliance by continuously monitoring technical safeguards. If it detects issues like misconfigurations, policy violations, or security gaps involving ePHI (electronic Protected Health Information), it sends alerts through email or ticketing systems. These alerts, paired with ongoing tracking of remediation efforts, ensure potential problems are addressed before they escalate into reportable breaches.
Automation of compliance processes
Censinet RiskOps™ takes automation to the next level by streamlining compliance workflows. It generates remediation plans based on questionnaire responses, assigns tasks to the right experts, and tracks progress for accountability. Its enterprise "roll-up" feature consolidates compliance data from various hospitals, clinics, and practices into a single dashboard, eliminating the manual effort of compiling reports across multiple locations.
Risk assessment and management capabilities
At its core, the platform maintains a centralized risk register and automates Security Risk Assessments (SRAs) across the organization. It simplifies compliance by centralizing documentation and policies, ensuring everything needed for audits is easily accessible. Additionally, it tracks vendor risk assessments, helping organizations evaluate the security measures of Business Associates and third-party vendors - an area often vulnerable in HIPAA compliance.
Audit readiness and reporting features
Censinet RiskOps™ also makes audit preparation seamless. Every action within the platform is recorded in an audit trail, creating a reliable repository for documentation, policies, and training materials tied to HIPAA safeguards. Real-time dashboards display compliance status across all HIPAA categories, while pre-built reports ensure organizations are always prepared for audits. This centralized approach simplifies the process, providing a clear, up-to-date view of compliance efforts.
2. Real-Time Alerts and Notifications
Immediate detection transforms compliance efforts by enabling a shift from reactive to proactive strategies. Real-time alerts continuously scan systems for potential compliance issues - like misconfigurations, policy violations, unauthorized access attempts, or encryption problems - and notify the right team members through channels such as email, Slack, or ticketing systems.
This shift from periodic audits to continuous monitoring changes how healthcare organizations manage HIPAA compliance. Instead of waiting for scheduled reviews, teams are notified instantly when issues arise with the safeguards protecting electronic protected health information (ePHI). These alerts track access logs, verify encryption status, and monitor activity controls to catch anomalies, such as unexpected workflow interruptions. The immediacy of these notifications integrates smoothly with automated workflows for remediation.
Automation takes this a step further by routing alerts through preferred communication channels and embedding them into existing workflows. Alerts configured to align with HIPAA controls use data masking to highlight urgency while keeping sensitive information secure. This approach minimizes manual oversight and turns compliance management into a continuous, day-to-day operation.
Real-time alerts also enhance risk assessments by dynamically updating centralized risk registers whenever vulnerabilities are detected. This triggers remediation workflows with clearly assigned tasks, ensuring compliance with HIPAA's Security Risk Analysis requirements. It also strengthens oversight of third-party risks, such as those involving Business Associates.
Every alert is logged with timestamps, creating a clear audit trail that simplifies compliance verification. Organizing these logs by HIPAA controls makes it easier for auditors to confirm that issues are resolved promptly, preventing them from escalating into reportable breaches or penalties.
3. Automated Evidence Collection
Automation of Compliance Processes
Manually documenting compliance processes can be a massive drain on time and resources - and it often leads to mistakes during audits. Automated evidence collection solves this by continuously gathering data like access logs, policy attestations, training completions, encryption proofs, and control validations. This eliminates the need for last-minute scrambling and shifts compliance from a periodic task to an ongoing process.
By connecting with tools like AWS, Azure, Google Drive, and HR platforms, the system automatically logs key compliance activities. For example, when an employee finishes HIPAA training or when access controls are updated, the software captures these events in real time. This means no more hunting for documentation during audits or investigations. Automated evidence collection acts like a real-time safety net, ensuring that compliance monitoring is always active. The result? Instant audit readiness becomes achievable.
Audit Readiness and Reporting Features
Once evidence is collected, the system organizes it according to HIPAA controls, making audit preparation straightforward. It generates auditor-ready reports that include dashboards, audit trails, and exportable logs. Each record is timestamped and securely stored, while the system highlights any missing or outdated entries, giving teams the chance to fix issues before they grow into bigger problems.
Additionally, PHI/PII masking automatically redacts sensitive information from system logs and reports. This ensures that audit trails remain thorough while still protecting sensitive data[6]. The system also logs every access and change to electronic health records, which is crucial for both compliance audits and investigations into suspicious activities[4].
Risk Assessment and Management Capabilities
The evidence collected doesn’t just sit there - it plays a key role in risk management. It feeds directly into risk registers and assessments, helping organizations evaluate ePHI risks, perform vendor assessments, and implement remediation strategies[3]. This proactive approach aligns with HIPAA's Security Rule[5], allowing organizations to go beyond basic compliance and focus on effective risk management.
4. Continuous Control Monitoring
Continuous control monitoring takes HIPAA compliance to a new level by making it an ongoing, proactive process.
Real-Time Alerts
With continuous control monitoring, security controls are tracked automatically and in real time across your organization’s systems. Instead of waiting weeks to uncover issues, these tools instantly flag problems like unauthorized access or encryption misconfigurations. Alerts are sent through platforms you already use - whether that’s Slack, email, or your ticketing system. You can even prioritize alerts by severity, ensuring critical threats are sent straight to your security team while less urgent issues are grouped for later review. This approach reduces alert fatigue and strengthens your ability to respond quickly to potential risks [2].
Automation of Compliance Processes
One of the standout benefits of continuous monitoring is its ability to automate compliance tasks. Advanced platforms scan your systems in real time, collect necessary evidence, and pinpoint misconfigurations or policy violations. By integrating with tools like cloud services, identity providers, and HR systems, these platforms keep a constant eye on safeguards such as data encryption, access controls, and activity logging. Real-time dashboards give you a clear picture of your compliance status, showing how quickly gaps are being addressed and how prepared you are for audits. Paired with real-time alerts, this automation ensures that HIPAA safeguards are consistently maintained [3].
Risk Assessment and Management Capabilities
Continuous monitoring also transforms risk management. Risk registers are automatically updated through real-time portfolio risk management as new threats emerge or controls are adjusted. With unified control frameworks, you can manage HIPAA requirements alongside other standards like SOC 2 and ISO 27001 - all from one dashboard. This real-time approach to evaluating risks to electronic protected health information (ePHI) means you’re no longer limited to annual assessments. Instead, you’re always one step ahead, addressing potential compliance issues before they escalate [3].
5. Risk Assessment Automation
Risk assessment automation is reshaping how healthcare organizations handle HIPAA Security Risk Analysis requirements. Instead of relying on manual spreadsheets, modern tools now utilize structured workflows to conduct thorough risk evaluations for both covered entities and business associates. These tools feature built-in rating systems that help identify, analyze, and prioritize risks to electronic protected health information (ePHI). What used to be periodic, manual audits has evolved into a continuous and more efficient process, seamlessly integrating with monitoring systems to ensure no compliance gaps are overlooked [3].
Automation of Compliance Processes
Automation takes the hassle out of compliance tasks by gathering evidence, identifying HIPAA-specific gaps, and assigning remediation tasks. Once a gap is flagged, the system generates an actionable plan that aligns with HIPAA Security Rule standards. These remediation tasks can then be assigned to subject matter experts within the platform, with real-time tracking tools that provide clear visibility into the status of each compliance issue.
Risk Assessment and Management Capabilities
Modern tools for risk assessment go a step further by dynamically updating risk registers as new threats emerge. They also simplify vendor risk management for Business Associates through automated assessments and renewal reminders [3]. Many platforms now offer unified control frameworks, allowing healthcare organizations to manage HIPAA requirements alongside other standards like SOC 2 and ISO 27001 - all from a single dashboard. Some systems even use a federated data model capable of mapping over 9,300 control statements to more than 1,200 regulations, including HIPAA, enabling advanced predictive risk analytics [7].
Audit Readiness and Reporting Features
Preparing for audits is far more efficient with automation. Cloud-based modules centralize all HIPAA-related documentation, including policies, training materials, handbooks, and certifications, linking each piece of evidence to specific safeguards [3]. These tools also timestamp records, ensuring they are audit-ready. By aggregating compliance data across various organizational units - whether hospitals, clinics, or departments - leaders gain instant insights into their overall risk posture, making it easier to address vulnerabilities and maintain compliance.
6. Centralized Policy and Procedure Management
Keeping track of HIPAA policies across an entire organization can feel like an uphill battle without the right tools. A centralized policy and procedure management system simplifies this by providing a single, secure location for all HIPAA-related documents, including Privacy and Security Rules and Breach Notification procedures. This setup eliminates the chaos of scattered files, outdated documents, and inconsistent access. It also ensures compliance stays on track while working seamlessly with automated risk monitoring systems.
Automation of Compliance Processes
Automation takes a lot of the stress out of compliance. With customizable HIPAA policy templates, you don’t have to start from scratch every time. These tools keep policies up-to-date and maintain a complete revision history. Automated workflows handle everything - from drafting and reviewing policies to distributing them and collecting employee acknowledgments.
Audit Readiness and Reporting Features
When it’s time for an audit, having all your documentation in one place can be a lifesaver. A centralized system keeps a detailed record of every policy's review, approval, and update, complete with timestamps and employee acknowledgments. This creates a clear audit trail that aligns with HIPAA’s Security Rule, covering the required administrative, physical, and technical safeguards. Instead of scrambling to find documents when auditors show up, compliance teams can quickly generate reports showing policy histories, attestation records, and the organization’s overall compliance status.
To stay ahead, healthcare organizations should look for tools that flag outdated policies automatically and link policy management with training modules. This ensures that staff are notified immediately when procedures change, creating a seamless cycle of policy updates and employee training.
7. Business Associate and Vendor Management
After conducting internal risk assessments, managing vendors and business associates becomes a crucial step in achieving HIPAA compliance. With 43% of healthcare breaches involving third parties[3], it's clear that organizations face significant challenges in tracking vendor access to PHI, keeping BAAs up to date, and ensuring third-party compliance with HIPAA standards. As internal controls become more automated, maintaining strong oversight of vendors is essential.
Risk Assessment and Management Tools
HIPAA compliance tools with automated risk assessment capabilities can transform how organizations manage vendors handling PHI. These tools use structured workflows and vendor questionnaires to assign risk scores automatically, creating a centralized vendor risk register. This register is separate from internal control assessments and helps organizations quickly identify vendors with the highest compliance risks. For example, platforms like Censinet RiskOps™ allow healthcare teams to assess vendor security, monitor PHI-related risks, and manage business associate relationships through collaborative workflows.
Streamlining Compliance Through Automation
Automation addresses many of the manual inefficiencies tied to vendor management. Advanced HIPAA tools simplify processes like BAA signing, sending renewal reminders before agreements expire, and automating onboarding questionnaires for new vendors. These systems ensure that signed BAAs are always accessible for audits and flag expired agreements for timely action. By tracking key details - such as contract dates, access permissions, and compliance documentation - automation can reduce administrative workloads by as much as 50%[3]. This not only simplifies daily operations but also provides a solid foundation for audit preparation.
Features for Audit Readiness and Reporting
When it's time for an audit, demonstrating proper management of business associates is critical. HIPAA compliance tools can generate detailed, audit-ready reports that include complete BAA logs, vendor risk scores, compliance evidence, and activity histories aligned with HIPAA controls. These platforms also maintain timestamps for all vendor interactions, creating a transparent audit trail that confirms continuous oversight. With real-time dashboards, organizations can monitor vendor compliance status at a glance, addressing any gaps before they escalate into audit issues.
8. Audit Trails and Reporting
Building on automated evidence collection and continuous monitoring, strong audit trails and real-time reporting ensure your HIPAA compliance efforts can be verified whenever needed.
Audit Readiness and Reporting Features
Detailed audit trails are at the heart of any effective HIPAA compliance tool. These systems meticulously log every user action and system change, creating a complete record that validates compliance with HIPAA's technical safeguards. This record not only demonstrates adherence to access control requirements, such as HIPAA session timeout rules, for electronic protected health information (ePHI) but also provides auditors with the evidence they need to confirm your organization's compliance efforts.
When it's time for an audit, audit-ready reporting tools save significant time and effort. Instead of spending weeks compiling data manually, these tools generate reports instantly. Top platforms organize evidence by control and framework, aligning directly with HIPAA Security Rule requirements[2][3]. Compliance officers can produce detailed reports that include policy histories, approval workflows, implementation timelines, and control effectiveness. These reports, backed by comprehensive audit trails, highlight continuous compliance oversight throughout the year.
Real-Time Monitoring and Alerts
Real-time dashboards simplify compliance management by consolidating data from multiple systems into one easy-to-read view. These dashboards combine audit trail information with compliance metrics, offering insights into incident status, policy adherence, and overall audit readiness[3][7]. By eliminating the need for manual data gathering, they transform HIPAA compliance from a periodic task into an ongoing, manageable process. For example, platforms like Censinet RiskOps™ provide a centralized hub where healthcare teams can monitor compliance in real time, spot gaps, and track progress on remediation efforts before issues grow.
Continuous control monitoring takes this a step further by integrating real-time alerts into the system. These alerts flag and document any control failures immediately, ensuring issues are addressed as they arise[3]. This ongoing monitoring not only strengthens your compliance stance but also provides auditors with evidence that control failures were identified and resolved promptly - a key factor in demonstrating a strong security posture[2].
Conclusion
Choosing the right HIPAA compliance tool is critical for safeguarding against serious risks. Data breaches in healthcare can lead to millions in losses, with fines reaching up to $25,000 per violation class [1][8]. Healthcare organizations face cyber threats at double the rate of other industries [8], making robust compliance measures even more essential.
To address these challenges, features like real-time alerts, automated evidence collection, continuous control monitoring, and audit trails are game-changers. These tools elevate compliance from a one-time task to an ongoing process. As symplr explains, "Manual and outdated procedures are unreliable and often prohibited for good reasons" [9]. Without automation, gaps in encryption, access controls, and vendor management can leave sensitive health information vulnerable.
When evaluating compliance tools, it's important to consider your organization's specific needs. Smaller practices may benefit from straightforward, budget-friendly options, while larger enterprises often require comprehensive, integrated platforms. Involve your IT team early to ensure compatibility with existing systems, and prioritize tools that include automated monitoring, real-time alerts, and secure Business Associate Agreements with full encryption for protected health information (PHI).
The move toward continuous, real-time monitoring isn't just a trend - it's the future of healthcare compliance. Investing in the right tools now means you're not just meeting regulations but also enhancing security, streamlining operations, and protecting patient data more effectively. In today's landscape, comprehensive compliance monitoring isn't optional - it's a necessity.
Censinet RiskOps™ provides continuous, automated monitoring to help healthcare organizations stay secure and compliant in an increasingly digital world.
FAQs
How can I tell which HIPAA controls a tool is monitoring?
To understand which HIPAA controls a tool monitors, focus on features such as audit logs, real-time alerts, and detailed reporting. These functionalities provide oversight and transparency regarding access to PHI or ePHI. For example, tools like Censinet RiskOps™ streamline evidence collection and combine real-time monitoring with audit preparation, offering a clear view of the controls being tracked. Ensure the tool monitors access logs, enforces security policies, and conducts risk assessments to maintain compliance.
What systems should a HIPAA monitoring tool integrate with first?
A HIPAA monitoring tool should work seamlessly with vendor risk assessment and continuous monitoring systems. This connection allows for real-time tracking of third-party compliance and security measures, which is essential for protecting patient data and adhering to HIPAA requirements.
How do these tools handle PHI in logs and audit reports?
HIPAA compliance monitoring tools play a critical role in safeguarding Protected Health Information (PHI) by maintaining tamper-proof logs of all activities involving PHI. These logs record essential details such as user identities, timestamps, actions performed, and transfer specifics.
To ensure data integrity, these tools often rely on techniques like cryptographic hashing or Write Once, Read Many (WORM) storage. Logs are typically retained for a minimum of six years, as required, and the system provides real-time alerts to flag any suspicious activity or anomalies.
By centralizing these logs, healthcare organizations can streamline audit preparation and confidently demonstrate compliance with HIPAA regulations. This not only enhances security but also simplifies the process of proving adherence to legal requirements.


