EHR Vendor Risk Assessment: Protecting Clinical Data and Ensuring System Reliability
Post Summary
An EHR vendor risk assessment must cover every system and service that interacts with patient data — not only the primary EHR platform but also patient portals, e-prescribing software, diagnostic and lab interfaces, billing systems, health information exchange connections, telehealth platforms, and backup systems — because mapping all these touchpoints is the prerequisite for identifying the full range of vulnerabilities that affect ePHI security.
HIPAA's Security Rule requires healthcare organizations to appoint a security officer, provide staff training, implement access controls, schedule regular assessments, maintain Business Associate Agreements for all vendors handling ePHI, and document all security measures — with HIPAA compliance responsibility resting with the healthcare provider rather than the EHR vendor regardless of contractual arrangements.
The five categories are security (data protection, authentication, incident response, disaster recovery), privacy controls (patient consent handling and access restrictions), availability and reliability (uptime guarantees, redundancy, and support response), interoperability (integration security with clinical tools), and compliance (HIPAA requirements, current certifications, and regular audits).
Vendors should be categorized using an evaluation matrix scoring them on security, compliance, data access, functionality, and credentials — with high-risk vendors flagged for detailed scrutiny based on factors including practice size, patient volume, specialty, and depth of system integration, ensuring that vendors handling sensitive ePHI receive the thorough assessment that their potential impact on patient care warrants.
EHR vendor contracts must mandate current data security measures, HIPAA and HITECH compliance, 21st Century Cures Act adherence, ONC-authorized certification, uptime guarantees of at least 99.9%, and robust disaster recovery and business continuity plans — with clear triggers for contract reviews and assessments scheduled at least 180 days before renewal.
Healthcare organizations that have automated third-party risk management have reduced PHI breach incidents by up to 60% compared to manual processes — with platforms like Censinet RiskOps™ providing real-time visibility into vendor compliance, security certifications, and emerging risks, enabling organizations to address issues proactively rather than discovering them after breaches have already occurred.
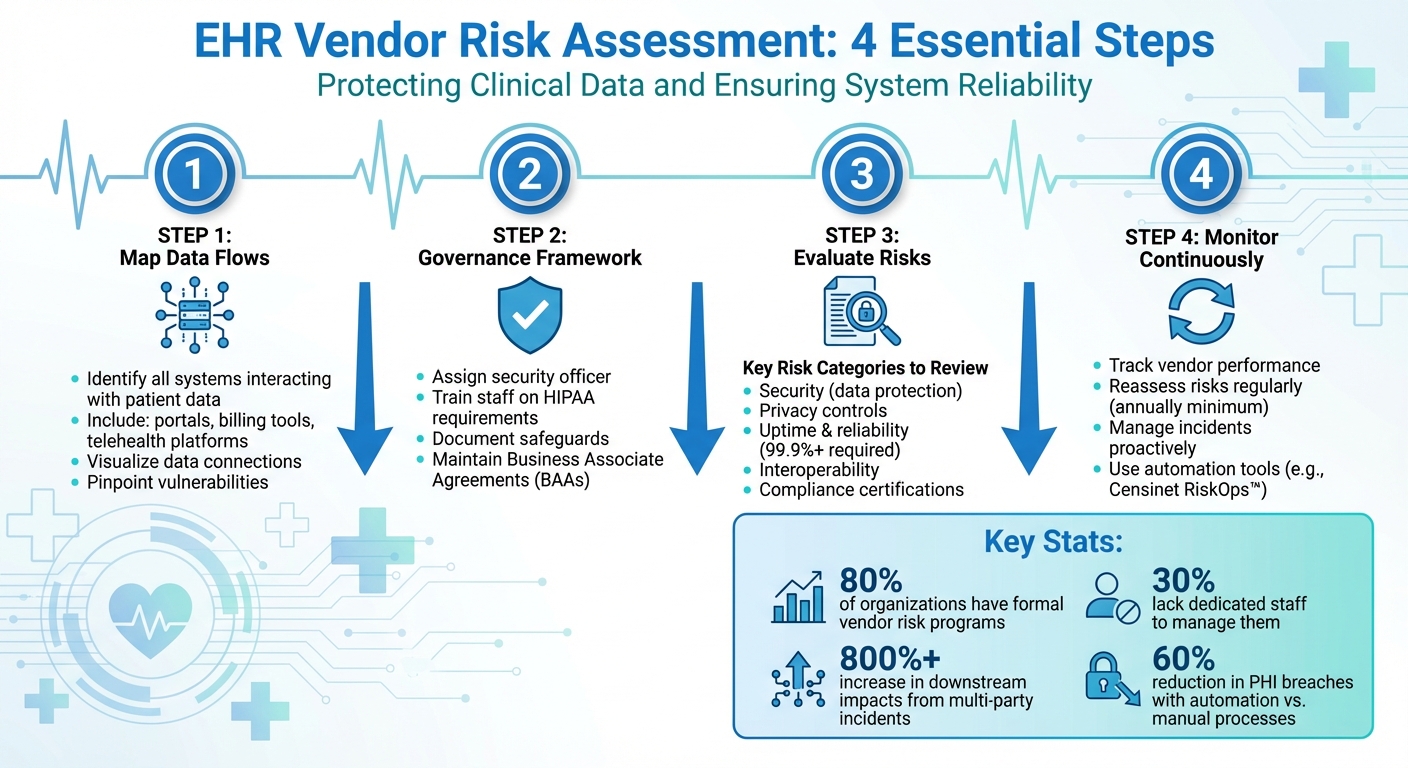
When choosing an EHR vendor, the risks tied to data security, compliance, and system reliability can’t be ignored. A single vulnerability in a vendor’s system could lead to data breaches, HIPAA violations, or disruptions in patient care. This guide simplifies the process of assessing EHR vendors by focusing on key steps:
4-Step
Process for Healthcare Organizations
Core Components of EHR Vendor Risk Assessment
Defining the Scope of EHR Vendor Risk
The first step in creating a strong vendor risk program is identifying every system and service that interacts with patient data. This goes beyond just your primary EHR platform. It includes related tools like patient portals, e-prescribing software, diagnostic and lab interfaces, billing systems, health information exchange (HIE) connections, telehealth platforms, and even backup systems. Mapping out these connections helps you visualize data flows and pinpoint vulnerabilities. Without a clear scope, hidden risks can easily slip through the cracks. Once you've mapped out all the touchpoints, you're in a better position to establish a governance framework that keeps everything secure.
Creating a Governance Framework
To protect electronic protected health information (ePHI), healthcare organizations need a solid governance framework guided by the HIPAA Security Rule. This framework should include administrative safeguards such as appointing a security officer, providing staff training, implementing access controls, and scheduling regular assessments. Proper documentation is also critical - this includes recording all security measures, maintaining Business Associate Agreements (BAAs), and outlining a plan for managing vendors who handle ePHI. It's important to note that while EHR vendors play a role in data security, they are not responsible for HIPAA compliance. That responsibility falls on healthcare providers. After completing a risk analysis, organizations should develop an actionable plan, which might involve updating software, adjusting workflows, revising policies, or conducting additional staff training [1].
Key Risk Categories to Evaluate
A thorough Security Risk Analysis (SRA) is essential for identifying vulnerabilities and putting safeguards in place. Once the governance framework is set, healthcare organizations should evaluate vendors across several critical risk categories to understand and mitigate potential threats:
Step-by-Step Process for EHR Vendor Risk Assessment
Vendor Intake and Classification
Start by identifying every vendor that interacts with your EHR environment. This means reviewing vendor agreements, contracts, and purchase orders to compile a complete inventory. Don't forget to include ancillary systems like patient portals, lab interfaces, and billing tools in this review [3]. Assign a security official to oversee the entire process and ensure you stick to a consistent risk evaluation methodology [4].
Next, categorize vendors based on risk factors such as the size of their practice, patient volume, specialty, and how deeply they're integrated into your systems [5][6]. To streamline this, use an evaluation matrix that scores vendors on key areas like security, compliance, data access, functionality, and credentials [5]. This approach helps flag high-risk vendors - especially those handling sensitive ePHI - for more detailed scrutiny.
Risk Analysis and Mitigation Planning
Once vendors are classified, dive deeper with a thorough risk analysis to uncover vulnerabilities. Assess each vendor's security protocols, privacy measures, system availability, interoperability, and compliance certifications [5][6]. Key areas to focus on include encryption methods, system uptime (aim for 99.9% or higher), disaster recovery plans, and certifications like HIPAA, HITECH, and the 21st Century Cures Act [5][6].
Document your findings and create a mitigation plan that addresses any gaps. This might involve requesting additional documentation, updating Business Associate Agreements, or implementing compensating controls. For vendors with significant risks, set clear timelines for remediation and assign follow-up responsibilities to ensure accountability.
After mitigation plans are set, stay proactive by monitoring vendors continuously and establishing robust incident management protocols.
Continuous Monitoring and Incident Management
Ongoing monitoring is crucial. Keep an eye on vendor performance by tracking metrics like uptime, adherence to service level agreements, and software updates that could introduce new vulnerabilities [5]. Establish clear escalation procedures and communication protocols for handling incidents [5][7]. For high-risk vendors, schedule regular reassessments - at least once a year - to evaluate changes in their security practices, financial stability, or compliance status. This ensures your EHR environment remains secure and compliant over time.
sbb-itb-535baee
Best Practices for EHR Vendor Risk Management
A structured risk assessment process is key to effective EHR vendor management. Here are some practical steps to help secure and simplify the process.
Standardizing Risk Assessments
Consistency is crucial when evaluating EHR vendors. While the HIPAA Security Rule doesn't prescribe a single method for risk analysis, it does require any chosen approach to meet specific objectives [2][1]. To ensure a reliable process, use established frameworks like NIST guidelines (SP 800-30, 800-66, 800-100, 800-115) for safeguarding electronic protected health information. The HITRUST Common Security Framework (CSF) is another helpful resource that ties existing frameworks to risk assessment and management [2].
Customized questionnaires are a great way to dig deeper into vendors' capabilities. Include questions on references, compliance, disaster preparedness, cybersecurity governance, and security controls [8]. For added support, organizations like the Healthcare Information and Management Systems Society (HIMSS) offer IT security self-assessment tools [2]. Tailor the depth of your assessments based on the vendor's role and importance.
"Risk is subjective - what one organization or industry can tolerate, another can't." - Jon M. Quigley, Principal, Value Transformation [8]
To streamline your evaluations, create a "perfect vendor" profile that reflects your organization's current and future needs. This profile can serve as a benchmark for future assessments and RFPs [8]. Use a consistent risk assessment matrix - like a 3x4 non-numeric scale for severity and likelihood - to evaluate threats and assign risk levels [8]. Document every step of the process, including data collection, identified threats, security measures, and risk level assignments [2].
Once a standardized approach is in place, automation can take efficiency to the next level.
Using Automation to Improve Efficiency
Manual oversight can be slow and prone to errors. By automating third-party risk management, healthcare organizations have reduced PHI breach incidents by up to 60% compared to manual processes [9]. This not only improves compliance but also enhances patient safety.
Censinet RiskOps™ is one tool that automates the entire workflow - from initial assessments to continuous monitoring. It offers real-time visibility into vendor compliance, security certifications, and emerging risks, ensuring you can address issues proactively [9]. The platform also lets you create tailored assessment templates based on vendor criticality and data access levels, streamlining the evaluation process through automated questionnaire distribution and response collection [9].
For even greater efficiency, Censinet AI™ accelerates risk assessments by allowing vendors to complete security questionnaires in seconds. It automatically summarizes vendor documentation, captures key integration details, identifies fourth-party risks, and generates risk summary reports. This blend of automation and human oversight shortens assessment cycles while keeping critical decisions in the hands of risk teams.
The platform’s advanced routing capabilities act like "air traffic control" for risk management, directing key findings and tasks to the appropriate stakeholders. With real-time data displayed in an intuitive dashboard, Censinet RiskOps™ becomes a centralized hub for managing AI-related risks, policies, and tasks.
While automation simplifies workflows, strong contracts remain a cornerstone of effective risk management.
Including Risk Requirements in Contracts
Your Business Associate Agreements (BAAs) and service contracts are your first line of defense. Embedding risk requirements in these agreements ensures that vendors uphold their responsibilities from the start.
Contracts should mandate that vendors implement up-to-date data security measures and comply with healthcare regulations like HIPAA, HITECH, the 21st Century Cures Act, and ONC-authorized certification bodies (ONC-ACBs) [5]. These certifications are non-negotiable for vendors handling clinical data.
Include an uptime guarantee of at least 99.9% to maintain high system availability [5]. Additionally, require vendors to have robust disaster recovery and business continuity plans to address potential outages [5]. These provisions create accountability and provide recourse if vendors fall short.
"The VRA doesn't stop once the vendor is engaged. Monitor for any variations in agreed-upon deliverables or processes." - Salma Suzie Fakhri, Owner and Director of FC2Y, Oceana 144 [8]
Set clear triggers for contract reviews, such as financial troubles, legal issues, or safety concerns [8]. Schedule regular reviews based on vendor risk levels: low-risk vendors might be reviewed annually, while high-risk vendors may need reviews twice a year or quarterly. Conduct a thorough review at least 180 days before contract renewal [8]. This ensures your agreements stay relevant as circumstances change.
Conclusion
Key Takeaways
Assessing the risks associated with EHR vendors is a critical step in safeguarding clinical data and ensuring system reliability. Recent statistics reveal that while nearly 80% of organizations have formal vendor risk assessment programs, around 30% lack the dedicated staff needed to effectively manage this responsibility [10]. This gap leaves organizations vulnerable to fines, lawsuits, financial losses, and damage to their reputation.
The ripple effect of multi-party incidents is staggering, with downstream impacts increasing by over 800% [10]. A striking example is the December 2022 breach involving Avem Health Partners and 365 Data Centers, which exposed the records of more than 271,000 patients [10]. This case highlights the reality that even a vendor’s security lapse can compromise patient data, regardless of how secure an organization’s internal systems might be.
Building a strong vendor risk program demands constant evaluation of all business partners. Taking a proactive approach - such as vendor classification, ongoing monitoring, and periodic reassessments - helps address potential issues before they escalate. Collaboration across departments like Compliance, IT, Security, Legal, and Finance ensures more thorough risk evaluations. Tools like Censinet RiskOps™ and Censinet AI™ bring automation into the mix, offering real-time insights into vendor compliance and emerging risks. These efforts collectively protect clinical data and enhance system reliability.
Next Steps for Healthcare Leaders
With these insights in mind, it’s time for healthcare leaders to take action. Start by reviewing your current vendor risk management practices and establishing a formal program with dedicated staff. Develop consistent criteria for evaluating vendor risks, ensuring that even vendors providing minor services are assessed, as they can still pose significant risks if they have access to sensitive data or physical spaces.
Classify vendors based on their risk level and the impact they have on your organization. For each vendor, create a detailed risk management plan that outlines specific responses, assigns responsibilities, and identifies mitigation strategies. Conduct assessments annually - or more often - to keep pace with changes in vendor operations and regulatory requirements. Regularly refine your criteria, methodologies, and tools to stay ahead of evolving risks [11]. Strengthening your vendor risk management program today will help protect patient data, improve system reliability, and ensure compliance with regulations in the long run.
FAQs
What are the essential elements of a successful EHR vendor risk assessment?
An effective electronic health record (EHR) vendor risk assessment focuses on a few essential elements to safeguard clinical data and keep systems running smoothly. These include assessing potential risks, keeping a close eye on vendor performance, ensuring adherence to regulatory requirements, and having a strong incident response plan ready to go.
It's equally important to prioritize continuous monitoring. This helps organizations catch and address vulnerabilities before they become serious issues. By concentrating on these areas, healthcare providers can protect sensitive patient information and ensure their systems remain dependable for delivering quality care.
How does Censinet RiskOps™ improve EHR vendor risk management?
Censinet RiskOps™ makes managing EHR vendor risks easier and more efficient by automating essential tasks like risk assessments and vendor evaluations. With its real-time monitoring capabilities, it ensures ongoing compliance tracking, enabling organizations to spot and tackle vulnerabilities as they arise.
By cutting down on manual work and enhancing precision, Censinet RiskOps™ helps healthcare providers safeguard sensitive clinical data while keeping their systems dependable.
Why is continuous monitoring essential for managing risks with EHR vendors?
Continuous monitoring plays a key role in managing risks associated with EHR vendors. It provides real-time insights into a vendor's security status, making it possible to spot potential vulnerabilities or threats early on. This enables swift action to safeguard sensitive patient information.
Beyond protecting data, continuous monitoring helps ensure the stability of essential systems. By addressing risks promptly, it minimizes the chances of disruptions in clinical operations, supporting both secure data management and uninterrupted patient care.
Related Blog Posts
- How to Conduct Effective Third-Party Risk Assessments
- Building Vendor Risk Frameworks for Healthcare IT
- EHR Vendor Risk Assessment: Protecting Clinical Data and Ensuring System Reliability
- Insurance and Benefits Administration Vendor Risk for Healthcare Organizations
{"@context":"https://schema.org","@type":"FAQPage","mainEntity":[{"@type":"Question","name":"What are the essential elements of a successful EHR vendor risk assessment?","acceptedAnswer":{"@type":"Answer","text":"<p>An effective electronic health record (EHR) vendor risk assessment focuses on a few essential elements to safeguard clinical data and keep systems running smoothly. These include <strong>assessing potential risks</strong>, keeping a close eye on vendor performance, ensuring adherence to regulatory requirements, and having a strong <strong>incident response plan</strong> ready to go.</p> <p>It's equally important to prioritize continuous monitoring. This helps organizations catch and address vulnerabilities before they become serious issues. By concentrating on these areas, healthcare providers can protect sensitive patient information and ensure their systems remain dependable for delivering quality care.</p>"}},{"@type":"Question","name":"How does Censinet RiskOps™ improve EHR vendor risk management?","acceptedAnswer":{"@type":"Answer","text":"<p>Censinet RiskOps™ makes managing EHR vendor risks easier and more efficient by automating essential tasks like risk assessments and vendor evaluations. With its <strong>real-time monitoring</strong> capabilities, it ensures ongoing compliance tracking, enabling organizations to spot and tackle vulnerabilities as they arise.</p> <p>By cutting down on manual work and enhancing precision, Censinet RiskOps™ helps healthcare providers safeguard sensitive clinical data while keeping their systems dependable.</p>"}},{"@type":"Question","name":"Why is continuous monitoring essential for managing risks with EHR vendors?","acceptedAnswer":{"@type":"Answer","text":"<p>Continuous monitoring plays a key role in managing risks associated with EHR vendors. It provides real-time insights into a vendor's security status, making it possible to spot potential vulnerabilities or threats early on. This enables swift action to safeguard sensitive patient information.</p> <p>Beyond protecting data, continuous monitoring helps ensure the stability of essential systems. By addressing risks promptly, it minimizes the chances of disruptions in clinical operations, supporting both secure data management and uninterrupted patient care.</p>"}}]}
Key Points:
Why must EHR vendor risk assessment extend beyond the primary EHR platform?
- The primary EHR is only one node in a complex clinical data ecosystem — patient portals, e-prescribing software, diagnostic and lab interfaces, billing systems, HIE connections, telehealth platforms, and backup systems all interact with ePHI and all represent potential attack vectors that a vendor risk program focused only on the EHR will miss
- The December 2022 Avem Health Partners and 365 Data Centers breach exposed the records of more than 271,000 patients — illustrating that even a vendor's data center infrastructure can compromise patient data regardless of how secure the organization's primary EHR implementation might be
- Multi-party incident downstream impacts have increased by over 800% — this statistic reflects the growing interconnection of healthcare vendor ecosystems, where a breach in one vendor relationship can cascade through integration points to affect patients and organizations far beyond the initial incident
- Telehealth platforms, mobile health apps, and cloud-hosted services significantly expand the attack surface — these systems often involve data flows that cross organizational and vendor boundaries in ways that traditional EHR-focused risk programs do not track, creating hidden ePHI exposure that only comprehensive scope definition can reveal
- Hidden risks slip through the cracks without complete scope mapping — organizations that assume their vendor risk program is comprehensive because it covers their EHR and major technology vendors consistently discover exposure in integration points, ancillary systems, and supporting infrastructure that full scope mapping would have surfaced earlier
What governance framework does HIPAA require for EHR vendor risk management?
- HIPAA's Security Rule requires appointing a security officer with oversight responsibility for the entire vendor risk assessment process — this is not an optional governance enhancement but a mandatory administrative safeguard under the Assigned Security Responsibility standard (§164.308(a)(2))
- Business Associate Agreements must be maintained for every vendor handling ePHI — these are not merely contractual formalities but legally required instruments that define permitted ePHI uses, require Security Rule compliance, and establish breach notification obligations for each vendor relationship
- HIPAA compliance responsibility rests with the healthcare provider, not the EHR vendor — understanding this distinction is essential because vendor contractual commitments do not transfer the organization's HIPAA obligations, and the healthcare provider remains accountable for ensuring vendor compliance through ongoing assessment and monitoring
- A complete risk analysis followed by an actionable remediation plan is required after governance framework establishment — the plan may involve updating software, adjusting workflows, revising policies, or conducting additional staff training, and its documentation is the evidence that demonstrates HIPAA compliance during regulatory review
- NIST guidelines and HITRUST CSF provide the recognized frameworks for structuring HIPAA-compliant risk analysis — using established frameworks ensures that the risk assessment methodology meets the regulatory standard for accuracy and thoroughness that HIPAA requires
How should healthcare organizations conduct EHR vendor risk analysis and prioritization?
- Vendor intake begins with a comprehensive inventory review — vendor agreements, contracts, and purchase orders must all be reviewed to compile a complete picture of every vendor interacting with the EHR environment, including ancillary systems that may not be obvious from the primary vendor relationship list
- An evaluation matrix scoring vendors on security, compliance, data access, functionality, and credentials provides the systematic prioritization framework that subjective risk judgment cannot — enabling organizations to direct assessment resources toward the highest-risk vendor relationships rather than assessing all vendors at the same depth
- Risk analysis must evaluate encryption methods, uptime targeting 99.9% or higher, disaster recovery plans, and certifications including HIPAA, HITECH, and the 21st Century Cures Act — with each assessment area generating documented findings that feed into the mitigation plan
- Customized questionnaires that include questions on compliance, disaster preparedness, cybersecurity governance, and security controls provide more actionable insight than generic vendor questionnaires — with assessment depth tailored to the vendor's role and importance in the clinical data ecosystem
- A perfect vendor profile reflecting the organization's current and future needs serves as a benchmark for assessment and RFP processes — creating a consistent standard that enables meaningful comparison across vendor relationships rather than evaluating each vendor against different implicit criteria
What does effective continuous monitoring look like for EHR vendor risk management?
- Continuous monitoring tracks vendor performance metrics including uptime, SLA adherence, and software updates that could introduce new vulnerabilities — replacing the point-in-time snapshot that periodic assessments provide with ongoing visibility into the vendor's actual security posture as it evolves
- High-risk vendors require reassessment at least annually with more frequent review when circumstances change — including new contracts, data-sharing agreements, mergers, significant software updates, or newly identified vulnerabilities that alter the vendor's risk profile
- Clear escalation procedures and communication protocols for incidents must be established before incidents occur — defining who is contacted, what information is required, and how remediation is tracked ensures that continuous monitoring translates into effective incident response rather than generating alerts that no one acts on
- Post-incident reviews must feed improvements back into the risk management program — root causes identified through incident analysis should update risk ratings, SLA requirements, and assessment criteria, creating a learning loop that strengthens the program over time rather than treating each incident as an isolated event
- Platforms like Censinet RiskOps™ and Censinet AI™ provide the automation infrastructure for monitoring at scale — real-time visibility into vendor compliance, security certifications, and emerging risks enables proactive issue resolution that manual monitoring at equivalent coverage would require prohibitively large compliance teams to maintain
How should contract risk requirements be structured for EHR vendor agreements?
- Contracts are the first line of defense in EHR vendor risk management — embedding specific risk requirements in BAAs and service contracts ensures vendors uphold their responsibilities before issues arise, rather than leaving remediation obligations ambiguous until an incident tests the contractual relationship
- Mandatory data security measures and HIPAA, HITECH, and 21st Century Cures Act compliance must be contractually required rather than assumed — ONC-authorized certification body certifications are non-negotiable for vendors handling clinical data and must be verified as current at contracting and at each renewal
- A 99.9% uptime guarantee establishes a measurable contractual baseline for system availability — with specific provisions for disaster recovery and business continuity plans that define how the vendor will restore operations in the event of an outage affecting clinical workflows
- Clear triggers for contract reviews — financial troubles, legal issues, safety concerns, or newly identified risks — prevent organizations from waiting until scheduled renewal to address material changes in vendor risk posture that arise between review cycles
- Reviews scheduled at least 180 days before contract renewal provide the lead time needed to negotiate improved terms, find alternative vendors if needed, or address compliance gaps without the leverage disadvantage that last-minute renewal negotiations create
What practical steps should healthcare leaders take to strengthen EHR vendor risk programs?
- Review current vendor risk management practices and establish a formal program with dedicated staff — the statistic that 30% of organizations with formal programs lack dedicated staff illustrates that program existence and program effectiveness are distinct, and only dedicated staffing produces the consistent assessment execution that genuine risk reduction requires
- Develop consistent risk criteria that cover even vendors providing minor services — minor vendors with access to sensitive data or physical spaces can still represent significant risks, and applying risk criteria uniformly prevents the systematic oversight gaps that result from assuming small vendors need less scrutiny
- Create detailed risk management plans for each vendor outlining specific responses, responsibilities, and mitigation strategies — generic program policies that are not translated into vendor-specific plans consistently fail at the implementation level where actual risk reduction happens
- Conduct assessments annually at minimum, or more often when vendor operations or regulatory requirements change — the pace of change in healthcare technology and regulation makes static assessment schedules increasingly inadequate for maintaining accurate vendor risk visibility
- Regularly refine criteria, methodologies, and tools to stay ahead of evolving risks — vendor risk programs that operate on fixed criteria become progressively less effective as the threat landscape and regulatory environment change, requiring systematic program review that updates assessment standards alongside emerging risk patterns


